Sperm Morphology 2%: What Does It Mean and How Can We Improve It?
Sperm Morphology & Its Impact on Fertility
As a fertility doctor, I meet many couples who feel very worried when they see a sperm morphology report of 2% or less.
Most men get shocked when they hear this number and start thinking they can never become a father. But the truth is, sperm morphology is just one part of semen analysis, and a report showing 2% does not always mean permanent infertility.
Let’s go step by step to understand what sperm morphology really means, when it is considered abnormal, and what can be done to improve your chances of conception.
What Is Normal Sperm Morphology?
Sperm morphology refers to the shape and structure of sperm. Under Kruger’s strict criteria, at least 4% of sperm must appear normal when examined under a high-power microscope (400x). This is considered the healthy threshold.
If less than 4% of sperm are consistently normal in two separate tests performed at least 20 days apart, only then is it considered to be teratozoospermia.
Sperm morphology of 2% means only 2 out of 100 sperm look normal, but this alone does not define infertility. We need to look at motility, count, and underlying causes.
Teratozoospermia and Related Conditions
Poor sperm morphology (teratozoospermia) condition often does not appear alone. Many times, men with teratozoospermia also have other sperm problems, such as
- Asthenozoospermia → low sperm motility (sperms that don’t move well)
- Oligospermia → low sperm count
- When all three problems—poor shape, poor movement, and low count—happen together, the condition is called oligoasthenoteratozoospermia (OATS).
Book Your Consultation Today With Dr. Jay Mehta—Fertility Specialist in Mumbai, India
Are All Reports of 1–2% Morphology Accurate?
One of the biggest challenges I see in India is incorrect reporting.
Many labs, especially those offering “free semen analysis” as part of IVF marketing, issue oversimplified one-page reports. These often declare “1–2% morphology” with low sperm count and poor morphology without following the proper WHO-recommended techniques.
Many of these patients come to us for a second opinion because we are well-known for our excellence in male fertility within our country.
From my personal experience, 95% of such reports are inaccurate. This creates unnecessary stress and confusion.
That’s why I always advise patients to repeat semen analysis in a reputable fertility clinic, with tests done at least 20 days apart.
When Poor Morphology Is Real: What Next?
If repeat reports consistently show less than 4% normal sperm, the next step is to understand the root causes of low sperm morphology (2% or less).
1. Lifestyle and Health Factors
The majority of patients improve significantly when we address:
- Stressful work profiles
- Unhealthy lifestyle
- Poor sleep
- Obesity, diabetes, hypertension
Lifestyle changes can reverse sperm morphology issues. With consistent effort, 50–70% of men see noticeable improvement within 4–6 months.
2. Clinical Examination
Most men with poor sperm morphology actually have normal testicular findings. This is encouraging because it shows the condition is often reversible with lifestyle changes.
3. Testicular & Genetic Factors
In 25–30% of cases, testicular factors play a role. These need deeper evaluation:
Sometimes, the cause lies in the testes themselves. Despite a normal physical exam, testicular dysfunction can cause persistent abnormal sperm morphology. Key genetic tests I recommend:
- Genetic testing
- Karyotyping
- Y-chromosome microdeletion
Both are simple blood tests, and results are usually available within 10 days.
4. Hormonal Imbalances
Hormones play a key role in sperm development. In cases of low morphology, we check:
- FSH
- LH
- Testosterone
- Estradiol
- TSH
- Prolactin
In most fertility centers, reports are available within 2–4 hours if in-house testing is present. These tests help us identify hidden testicular issues that may affect sperm quality. Correcting these imbalances often improves sperm quality.
It’s important to understand that when the problem comes from the testicles, we need to carefully sit down with the patient and identify exactly what is wrong with the sperm.
A detailed sperm analysis often shows that the issue may be in the head of the sperm, sometimes in the neck, or even in the tail. In some men, more than one part of the sperm is affected at the same time.
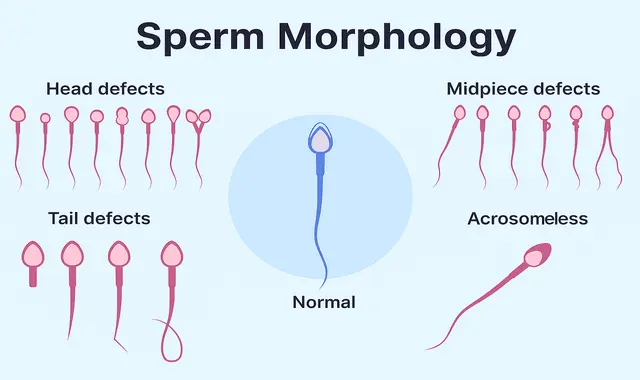
Types of Abnormal Sperm Defects Seen in 2% Morphology
Based on where the problem lies, different abnormalities can be seen in sperm:
- Head defects—These are among the most serious problems because the sperm head carries the genetic material and enzymes needed to enter the egg. When the head is abnormal, fertilization becomes very difficult. Common head problems include:
- Giant heads
- Pinheads
- Acrosomal defects (the cap that helps sperm enter the egg is missing or abnormal)
- Globozoospermia—where the head is round and unable to fertilize the egg naturally
- Neck defects—If the neck is bent or irregular (often called a “bent neck”), the sperm cannot move properly. This reduces motility and leads to very low fertilization rates.
- Tail defects—The tail is what propels the sperm forward. If the tail is short, coiled, or missing, motility becomes extremely poor, making it nearly impossible for sperm to reach the egg.
In many men, we see a combination of head, neck, and tail defects in the same semen sample.
Unfortunately, these abnormalities interfere significantly with natural conception methods like timed intercourse or even IUI (Intrauterine Insemination), which rely on the sperm swimming to the egg.
How to Improve Sperm Morphology from 2%?
The approach depends on the underlying cause. Here’s the structured way I manage patients:
Step 1: Lifestyle & Habits
- Improve sleep cycle
- Reduce stress
- Exercise and maintain healthy weight
- Avoid alcohol, smoking, and drugs
Step 2: Medical & Hormonal Therapy
- In carefully selected men, recombinant FSH injections given 3 times a week for 12–16 weeks can improve sperm quality.
- For men with a testosterone-to-estradiol (T/E) ratio >10, I sometimes prescribe Letrozole on alternate days for added benefit.
Step 3: Assisted Reproduction Options
- IUI (Intrauterine Insemination): Usually not effective in men with severe teratozoospermia.
- ICSI (Intracytoplasmic Sperm Injection): A standard procedure where a single sperm is injected into the egg.
- IMSI (Intracytoplasmic Morphologically Selected Sperm Injection): An advanced technique where sperm are examined under 6000x magnification to choose the best ones.
From my own experience, IMSI helps us select healthier sperm under very high magnification.
This often results in better embryo quality and the development of more blastocysts compared to standard ICSI.
However, I always explain to couples that pregnancy rates with IMSI are not dramatically higher than with ICSI.
Step 4: Genetic Testing of Embryos
For couples where sperm morphology remains poor despite interventions, I recommend Preimplantation Genetic Testing (PGT) before embryo transfer. This helps us identify chromosomal abnormalities early and improves chances of a healthy pregnancy.
It is also important to know that IMSI cannot guarantee fertilization success. This is especially true in cases of severe head defects, such as globozoospermia, where sperm struggle to fertilize the egg even under ideal conditions. In such situations, I strongly recommend doing genetic testing of embryos (PGT) before transfer. This allows us to identify the healthiest embryos and improves the chances of a safe and successful pregnancy.
Does IMSI Help More Than ICSI in Poor Morphology?
IMSI allows us to study sperm at a very high magnification of 6000x, which makes it possible to choose the healthiest-looking sperm for fertilization. This often leads to better-quality embryos and a higher number of blastocysts compared to standard ICSI.
However, both medical studies and my own practice show that IMSI does not significantly increase overall pregnancy rates when compared to ICSI.
In my experience, I usually recommend IMSI for men with persistently poor sperm morphology, because it helps me make the most accurate sperm selection.
At the same time, I am always honest with couples: IMSI is not a guarantee of pregnancy. What it can reliably offer is the chance to create stronger embryos, which gives us a better foundation to work with during treatment.
My Clinical Experience With 2% Sperm Morphology Patients
- Most patients with lifestyle-related issues show clear improvement after 4–6 months.
- Patients with globozoospermia usually have the poorest outcomes with their own sperm.
- A large number of patients come to me with incorrect reports, which unnecessarily worsens their anxiety.
This is why accurate diagnosis and timely treatment are key.
We are very fortunate to be a referral center for male fertility disorders in India, which allows us to see and support a large number of patients from across the country. Many of them connect with us through online consultations and virtual counseling, and I am glad to share that a significant number are able to receive the right guidance and effective management without needing to travel.
📞 If you or your partner are struggling with male infertility, you can connect with us directly at 1800-268-4000 for expert advice and compassionate support.
Do Ayurvedic or Homeopathic Medicines Improve Sperm Morphology?
I want to be very clear—there is no scientific evidence that Ayurvedic or homeopathic medicines can improve sperm morphology.
Sadly, I see many men in India lose valuable reproductive time while trying these unproven treatments. By the time they return to us, their chances of success are often reduced. My strong advice is to avoid unscientific therapies and focus only on evidence-based treatments that are proven to help.
Hormonal Treatment for Low Sperm Morphology and Male Infertility
At this point, I also want to address a smaller group of men who fall into what we call Aphrodite criteria 4 or 5—meaning they may have unexplained male infertility or infertility due to testicular insufficiency.
In carefully selected patients like these, we sometimes recommend hormonal treatment.
One option is recombinant FSH injections, given in low doses three times a week (3 times/week) for about 12 to 16 weeks.
In some men, this can lead to noticeable improvement—but only if their testosterone levels are close to normal and their FSH levels are normal or only slightly raised.
Another important measure we look at is the T/E ratio (testosterone-to-estradiol ratio). If this ratio is greater than 10, we often add Letrozole on alternate days to improve outcomes.
Of course, deciding on hormonal treatment requires a detailed hormonal evaluation of each male patient. This step ensures that the right men get the right therapy without unnecessary medication.
I truly hope this explanation helps men facing poor sperm morphology understand their condition better. My goal is always to provide clear, evidence-based guidance so you can make the right decisions with confidence—not based on myths or hearsay, but on science and experience.
Key Takeaways
- A report of sperm morphology of 2% should never be accepted at face value—always retest in a reputable fertility center.
- Lifestyle modifications (stress reduction, weight loss, better sleep, and managing diabetes/hypertension) can improve sperm quality in 50–70% of men.
- If lifestyle doesn’t help, investigate genetic and hormonal causes.
- ICSI/IMSI offer the best fertility outcomes in severe morphology cases.
- Avoid falling into unscientific therapies that waste time
As a fertility expert, I want to reassure you:
Poor sperm morphology is not the end of the road.
Most men can see improvement with the right lifestyle changes, medical evaluation, and personalized treatment plan.
If needed, advanced techniques like IMSI and embryo genetic testing give us powerful tools to achieve pregnancy safely.
If you or your partner have been told you have sperm morphology of 2% or less, don’t panic. Seek a second opinion at a specialized fertility clinic, get the right tests done, and let us guide you toward the most effective treatment.
Dealing with male infertility can feel overwhelming, but you are not alone. With the right diagnosis, lifestyle changes, and advanced treatments like ICSI, IMSI, and embryo genetic testing (PGT), many couples achieve their dream of parenthood.
If you’ve been told you have low sperm morphology (2% or less) or are struggling with repeated IVF/ICSI failures, I encourage you to reach out. Together, we can find the most effective, evidence-based treatment tailored to your situation.
📞 Call us today at 1800-268-4000 to book your consultation and take the first step toward building your family.
Frequently Asked Questions on Sperm Morphology
– What does sperm morphology 2% mean?
When a semen analysis shows 2% sperm morphology, it means only 2 out of 100 sperm appear normal under strict Kruger criteria. If less than 4% of sperm are normal on two separate tests, this is called teratozoospermia.
– Can sperm morphology improve naturally?
Yes, in most men, sperm morphology can improve with simple lifestyle changes.
- Reducing stress
- Improving sleep quality
- Maintaining a healthy weight
- Managing diabetes or hypertension
- Avoiding smoking and alcohol
With these steps, 50–70% of men notice improvement within 4–6 months.
– What causes poor sperm morphology?
There are two main reasons:
- Lifestyle-related factors: stress, obesity, poor sleep, and unhealthy habits.
- Medical causes include genetic abnormalities (Y-chromosome microdeletion, karyotype issues), hormonal imbalance, or testicular dysfunction.
– Is 2% sperm morphology dangerous?
No, it doesn’t harm a man’s overall health. But it can lower natural fertility chances. When sperm morphology is severely poor, natural conception or IUI may fail—and advanced fertility treatments like ICSI or IMSI may be recommended.
– Should I repeat the test?
Yes. Always repeat semen analysis at least 20 days apart in a reputable lab.
– What tests should I do if my morphology is 2%?
Repeat semen analysis, karyotyping, Y-chromosome microdeletion, and a complete hormonal profile.
– Can vitamins or supplements fix poor morphology?
Supplements may support sperm health, but lifestyle and medical corrections are far more effective.
– What foods help sperm morphology?
Antioxidant-rich foods like nuts, berries, vegetables, and whole grains can support sperm health.
– Do Ayurvedic or herbal medicines help?
No. There is no scientific proof. They only delay effective treatment.
– Which treatment helps in low sperm morphology?
- First step: Correct lifestyle factors
- Next step: Hormonal and genetic testing if needed
For fertility treatment: ICSI or IMSI are the best options, as they allow embryologists to select the best possible sperm under high magnification.
– Is IMSI always better than ICSI?
Not always. IMSI helps with better sperm selection and embryo quality but does not guarantee higher pregnancy rates.

Dr. Jay Mehta
MBBS, DNB—Obstetrics & Gynecology
IVF & Endometriosis Specialist, Laparoscopic Surgeon (Obs & Gyn)
Dr. Jay Mehta is a highly renowned IVF specialist and fertility-preserving surgeon based in Mumbai, India. As the director of the Shree IVF and Endometriosis Clinic, Mumbai, he is recognized as one of India's leading laparoscopic gynecologists for the advanced treatment of complex conditions such as endometriosis and adenomyosis.
Dr. Mehta's expertise extends deeply into reproductive medicine; he is a well-known IVF specialist and among the few practitioners in the country with specialized knowledge in embryology, andrology, reproductive immunology, and Mullerian anomalies. Dr. Mehta conducts operations and consultations across India's major cities, including Pune, Chennai, Hyderabad, Bangalore, Ahmedabad, Agra, and Delhi. To book an appointment, call: 1800-268-4000
Blogs

How Common is Male Infertility?
If you’re dealing with infertility, don’t feel alone – you’re far from it. And if you’re wondering how common male infertility is, read the latest statistics

Is Azoospermia the same as Aspermia?
Aspermia results in complete lack of ejaculation in men, while azoospermia results in no sperm in the ejaculate
Videos

Does Azoospermia Surgery Affect Sex Life?
Will azoospermia surgery change your sex life? In most cases, no. Understand the benefits of the procedure and how it can help restore fertility

Causes and Treatment of Non-Obstructive Azoospermia
Nonobstructive Azoospermia means no sperm in the ejaculate. It can be caused by genetics, hormones, testicular failure, or ejaculation issues



