Home » Fertility » Azoospermia » Non-Obstructive Azoospermia
Non-Obstructive Azoospermia
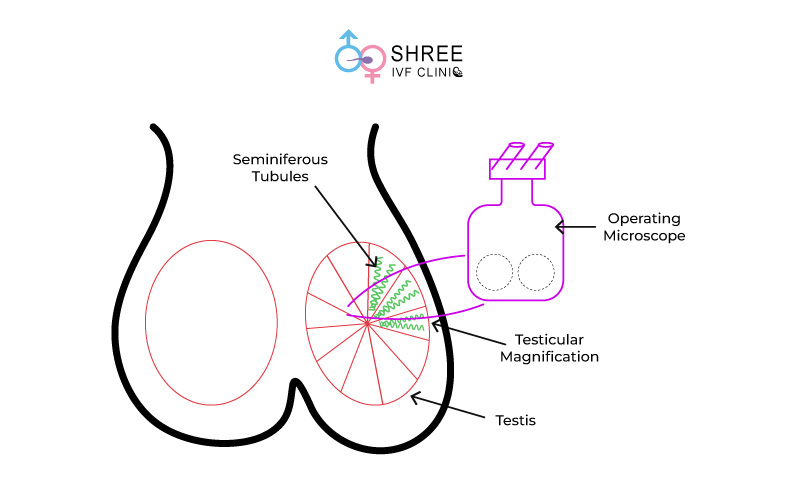
Male infertility is an increasingly recognized health issue, with non-obstructive azoospermia being one of its most severe forms.
Non-Obstructive Azoospermia is characterized by the absence of sperm in a man’s ejaculate due to a failure of spermatogenesis.
This condition presents unique challenges for both the affected individual and their partner, often necessitating specialized care and treatment.
What is Non-Obstructive Azoospermia?
Non-Obstructive Azoospermia is a type of azoospermia where there’s no sperm in the ejaculate because of a problem with sperm production.
It’s different from obstructive azoospermia, which is caused by a blockage in the reproductive tract that prevents sperm from reaching the ejaculate.
Causes of Non-Obstructive Azoospermia
The causes of Non-Obstructive Azoospermia are varied and can include genetic abnormalities, hormonal imbalances, testicular injury, or even undetermined factors.
Some men may have Non-Obstructive Azoospermia due to a history of testicular cancer or because they’ve undergone treatments like chemotherapy or radiation, which can affect sperm production.
Other men may have Non-Obstructive Azoospermia due to genetic anomalies, such as Klinefelter syndrome or Y chromosome microdeletions.
Symptoms of Non-Obstructive Azoospermia
Most men with NOA won’t have any signs or symptoms and may not even realize they have a fertility issue until they attempt to conceive.
However, some men may experience certain symptoms associated with their underlying cause, such as pain, swelling or difficulty in urinating. It’s important to speak with your doctor if you’re experiencing any of these issues
The primary sign of Non-Obstructive Azoospermia is azoospermia, which means that no sperm are found in the semen when it’s examined under a microscope.
Other possible signs include small, soft testes or testicular microlithiasis, which involves the presence of tiny, hard lumps of calcium inside the testicles.
Book Your Consultation Today With an Azoospermia Specialist in Mumbai India – Dr Jay Mehta
Diagnosis of Non-Obstructive Azoospermia
Diagnosis of Non-Obstructive Azoospermia usually involves several steps, beginning with a semen analysis to confirm the absence of sperm.
The doctor may then order additional tests to determine the underlying cause. These can include genetic tests, hormone levels, a testicular biopsy or imaging studies like ultrasound or MRI.
Once the underlying cause is determined, the doctor will be able to develop an individualized plan of care tailored to your needs. This could involve medications, lifestyle changes
Hormonal testing might be performed to check levels of testosterone and other hormones involved in sperm production.
In some cases, a testicular biopsy may be needed to determine whether there’s a problem with sperm production or if there’s a blockage preventing sperm from reaching the ejaculate.
Treatment Options for Non-Obstructive Azoospermia
Treatment options for Non-Obstructive Azoospermia tend to focus on assisted reproductive technology (ART), such as in vitro fertilization (IVF) or intracytoplasmic sperm injection (ICSI).
These treatments involve extracting sperm from the testes, either directly or from extracted tissue, and then using it to fertilize a woman’s egg in a laboratory.
In some cases, fertility drugs may be used to stimulate sperm production. Other options include microdissection testicular sperm extraction (microTESE), which involves surgically removing
It’s important to note that Non-Obstructive Azoospermia isn’t always treatable, and the likelihood of success depends on its underlying cause.
Regardless, a fertility specialist can work closely with you to develop an individualized treatment plan tailored specifically to your needs.
With the right approach and support, you can increase your chances of achieving a successful pregnancy.
Choosing the right doctor for endometriosis treatment is of utmost importance. The impact it can have should never be underestimated, it can truly make a significant difference. Dr. Jay is a very experienced fertility & one of the best azoospermia doctor in Mumbai.
Conclusion
Non-Obstructive Azoospermia is a complex condition with a variety of potential causes and treatments. It’s crucial to work closely with a healthcare provider to develop a personalized treatment plan.
Understanding the genetic basis of Non-Obstructive Azoospermia could help inform treatment strategies and provide valuable information for family planning. Recent research has started to shed light on promising new treatments for Non-Obstructive Azoospermia, including the use of stem cell therapy.
The emotional impact of Non-Obstructive Azoospermia cannot be overlooked, with many men experiencing feelings of stress, depression, and anxiety. Support groups can provide a safe space for men and their partners to share their experiences, gain information, and find comfort in knowing they’re not alone.
FAQ’s
– Is non obstructive azoospermia more common than Obstructive Azoospermia?
Yes definitely, non obstructive azoospermia, the most common cause for Azoospermia. About 85% of total cases are Non Obstructive and about 10-15% are due to Obstructive causes.
– Is it compulsory for hormonal parameters to be abnormal in patients with non obstructive Azoospermia?
Typically we analyze FSH and LH and testosterone. In some cases based on clinical examination estradiol is also recommended. Most of the situations one can have elevated values of FSH.
Simultaneously it is also important to assess if the value of testosterone is more than 350 or not. Ratio of testosterone to Estradiol is important, especially in patients who are obese.
– Can patients having non obstructive azoospermia be treated with medical management?
Medical management is typically beneficial only and only for two patients who are having proven hypogonadotropic hypogonadism. It is the patients who typically require a prolonged course of injectables, these injectables are typically given for a span of 12 to 18 months.
Typically HMG and HCG injections are administered to the patient. Only in this case one may have a variable benefit on the sperm count. Have a word many of these males ultimately require, either IUI or IVF.
– Why is it that an expert should perform microTESE?
MicroTESE is considered to be the standard therapy of choice for a patient having non-obstructive Azoospermia.
According to regulations it should ideally be an andrologist or a team of andrologists and a highly skilled gynecologist performing the procedure, at our institute we follow a very specific technique for doing this. It is the urologist who comes and opens the testis, following which microscopic examination inside the testis is performed individually and personally by Dr Jay Mehta.
This allows him to specifically identify the high probable zones (HPZs), inside of the testis in order to accurately determine tubules which are having sperm production. Distributes are delicately defected out and her personally examined inside the laboratory.
Once sperms are retrieved, the female partner is called inside the laboratory to show the sperms of the male partner. The urologist then carefully closes the testis.
This allows Dr Mehta to obtain an extremely high amount of sperm retrieval rate even in extremely complicated cases. This is the only unit in the country where a combination of a urologist and highly skilled fertility specialist are adapted in performing the procedure right from sperm retrieval to sperm processing two performing of any other fertility procedure which may be indicated.
– How much is the recovery period after microTESE?
When done correctly this is a highly effective procedure for the male partner. This procedure takes approximately 2 hours to perform. Following this the male partner can resume all the activity on the next day of the procedure.
– What is the type of Anesthesia used for doing microTESE?
There are a lot of males who will be able to tolerate this entire procedure under local anesthesia + sedation.
However in certain situations general anesthesia can also be administered to the male partner based on requirement.
– Is it compulsory for only Urologists / Andrologist to perform microTESE?
According to the assisted reproductive technology act in India either a urologist or a General Surgeon or a highly skilled gynecologist in reproductive medicine can perform the procedure for microTESE.
However it is extremely important to understand that in such a type of critical surgery, it is the experience of the treating doctor, which makes a massive outcome benefit in the sperm retrieval rate.
Dr Jay Mehta and his team hold the credit for performing the maximum number of these surgeries in India.
– How much is the sperm retrieval rate following the procedure for microTESE?
The average sperm retrieval rate for microTESE is going to be between 55 to 60%. However for certain indications like post chemotherapy, viral orchitis, undescended Testis, secondary gonadal failure post trauma, the sperm retrieval rates could be much lesser.
Even if the level of testosterone is less than 350, the probability of retrieving sperm successfully would become less than 30%. At our unit we normally provide the sperm retrieval rate to the patient in writing.
Dr Jay Mehta and team firmly believe in the policy of not over promising results to the patient.
– Can a patient have routine sexual life and intercourse after undergoing microTESE?
The patient can have a routine sexual life and sexual intercourse. The procedure does not affect the sexual function in any manner. After 2 weeks of the procedure, the patient can easily resume sexual intercourse.
– Do these patients need any form of pre-medicines to increase the sperm Retrieval Rate in Non Obstructive Azoospermia?
Apart from cases which have specifically documented hypogonadotropic hypogonadism, the role of any form of oral tablets or injections in the patients is extremely negligible.
Though it may allow the patient to buy time in order to become mentally ready for the procedure, the overall outcome in enhancing sperm retrieval rates has not been established.
– Can any form of alternative therapy benefit these patients who have Non Obstructive Azoospermia?
The commonest patient behavior is to jump or switch to an alternative medicine, once they initially recommended surgery. However none of the alternative therapy approaches has ever been proven to benefit the patients.
Before jumping on to any of these therapies, patients are strongly advised to do their own research and take it in writing from the treating specialist regarding the successful outcome of their proposed therapy.
– Does Varicocele Surgery enhance sperm Retrieval Rate in Non Obstructive Azoospermia?
Varicocele surgery is one of the most commonly abused surgeries. There is no add on benefit of doing this surgery in increasing the sperm retrieval rate.
Unless there is a large varicocele, which is typically associated with testicular pain, one may perform the surgery in order to reduce the pain in the testis.
– Is there any role at the moment of Stem Cell Therapy in curing Non Obstructive Azoospermia?
At the moment stem cell therapy in patients is considered to be of experimental and research phase for Azoospermia. For this therapy to become a clinical success, it may be another 4 to 6 years away.
– Can a change in diet cure Non Obstructive Azoospermia?
Changing the diet or switching to a healthy diet has got no added benefit in treatment and cure for non obstructive Azoospermia.
– Why is it difficult to mentally accept the condition of Azoospermia?
In this condition most of the time the external appearance and physical features of the male partner are absolutely normal. Simultaneously there is no problem in performing sexual intercourse or masturbation.
As a result of this acceptance of this condition can be pretty challenging for the male partner. From our experience a male partner once diagnosed typically takes 18 to 24 months prior to performing definitive therapy for this condition.
This is also limited by various other regional factors, social factors and cultural factors which exist in India.
– What are the LIVE Birth rates for Non Obstructive Azoospermia following microTESE?
The life birth rate following this procedure comes to approximately 20%. Due to common marketing practices of IVF clinics, a patient often gets misguide dead by unrealistically high promises of success rates.
– Is taking Donor sperms the ONLY option for Non Obstructive Azoospermia?
More than 55 to 60% of mails who have this condition can be blessed with a child using their own sperm.
Patients are encouraged to do their research and go to the doctors who are experts in performing this procedure so that they have the best chance of getting their own genetic child.
– Does microTESE require any special instruments?
Yes this procedure is typically done on an operating microscope. This instrument is expensive and it allows for optimal magnification, in order to correctly identify the high probable zone (HPZ), which then provides for the best sperm retrieval.
– Are sperms obtained from microTESE healthy?
Yes yes, the sperms that are typically obtained from the healthy tubule are healthy sperms. These forms could have slightly lower motility, however if proper selection of sperm is done it offers for excellent fertilization rates, excellent blastocyst formation rates, and excellent clinical pregnancy outcome.
– Is microTESE an expensive procedure?
The expense of any surgery is decided upon the facility available in the premises and the available expertise of the medical team.
– Is it mandatory to do a Genetic Testing Prior to Surgery for Azoospermia?
After doing a clinical examination of the patient, if it is mandatory then a standard karyotyping along with Y chromosome microdeletion, may be recommended to the patient.
It is important to note that if we are testing for Y chromosome microdeletion, then AZFc is the only favorable mutation. If the patient has tested positive for a Y chromosome microdeletion, strong recommendation for performing genetic testing is done.
– Are there chances of sperm retrieval in cases of testicular failure?
NO. Patients who are into testicular failure have virtually no hope of retrieving sperms, this is mainly because extremely low values of testosterone majority of these patients will require testosterone replacement therapy at some point in time.
– Is there any chance of sperm retrieval in cases of Klinefelter Syndrome?
Though the FSH value is extremely high, in these cases and the size of the testis is extremely small, surprising these patients still have a 5% sperm retrieval rate.
– After how long following chemotherapy can one attempt microTESE?
Usually any form of chemotherapy which is administered to the patient has a detrimental effect on the sperm production. Majority of the specials end up with non obstructive Azoospermia.
Ideally after the completion of 3 years of chemotherapy, one can attempt any of the sperm retrieval procedures, but one must note that in these cases the chances of retrieving healthy sperm is going to be approximately 10 to 15%. The sperm retrieval rate after radiation therapy is virtually absent.
– Can a correction of Undescended Testis enhance Sperm Retrieval rate?
Patients who are having an undescended testis, will usually present with Azoospermia. Corrective surgery for undescended testis is ideally to be attempted within the first 2 years of birth.
This could be a multi stage procedure. However if somebody attempts this procedure after adolescence, it virtually has negligible NO effect on enhancement of sperm retrieval rate.
In some types of rare situations, one May recommend surgery in order to reduce the possibility of development of testicular cancer.
– Can the Sperm which is obtained through microTESE be stored or Frozen?
There are various techniques which exist for testicular sperm freezing. One of the commonest techniques which is followed is preservation or freezing of the entire testicular tubule.
Slightly Newer method involves freezing of the sperm in a specialized device called as sperm VD.
This device allows for freezing of individualized sperm. Dr Jay Mehta and team have achieved many many successful pregnancies with the help of these techniques.
The team has to its credit one of the first live births after freezing of just a single sperm in the sperm VD device.
– Is there a risk that the child born through microTESE can also have Azoospermia?
NO. There is no such risk that has been proven. This type of risk can only exist if there is a genetic abnormality, as has been discussed above. A prospective parent should not get scared, and should not keep this type of thought in their mind.
– What are the complications of doing a microTESE?
A few of these males can experience a testicular hematoma or a testicular infection provided the surgery is not done using the correct technique. These complications are then usually managed conservatively.
– Which is the microscope used by Dr Jay Mehta for doing microTESE?
Labomed prima 3 axis operative microscope.

Dr. Jay Mehta
MBBS, DNB—Obstetrics & Gynecology
IVF & Endometriosis Specialist, Laparoscopic Surgeon (Obs & Gyn)
Dr. Jay Mehta is a highly renowned IVF specialist and fertility-preserving surgeon based in Mumbai, India. As the director of the Shree IVF and Endometriosis Clinic, Mumbai, he is recognized as one of India's leading laparoscopic gynecologists for the advanced treatment of complex conditions such as endometriosis and adenomyosis.
Dr. Mehta's expertise extends deeply into reproductive medicine; he is a well-known IVF specialist and among the few practitioners in the country with specialized knowledge in embryology, andrology, reproductive immunology, and Mullerian anomalies. Dr. Mehta conducts operations and consultations across India's major cities, including Pune, Chennai, Hyderabad, Bangalore, Ahmedabad, Agra, and Delhi. To book an appointment, call: 1800-268-4000
Blogs
How Long Can Sperm Live Inside the Female Body?
Sperm survive up to 5 days in fertile mucus, average 3 days. Outside the body, they die within minutes or up to 30 minutes in moist conditions

Reasons for Not Getting Pregnant When Everything is Normal
You may not get pregnant despite trying due to unexplained infertility, hidden sperm or egg issues, implantation failure, or immune factors
Videos

Ovarian Stem Cell Transplant (Age 40-50): Does It Work?
Stem cell ovarian transplant may help restore fertility and hormone levels in women 40-50, but its effectiveness remains under clinical research

Autologous Stem Cell therapy in IVF & Infertility Treatment
Autologous Stem Cell Therapy offers hope for women with low AMH and thin endometrium, improving IVF outcomes for those facing early fertility issues



