Vaginal Agenesis
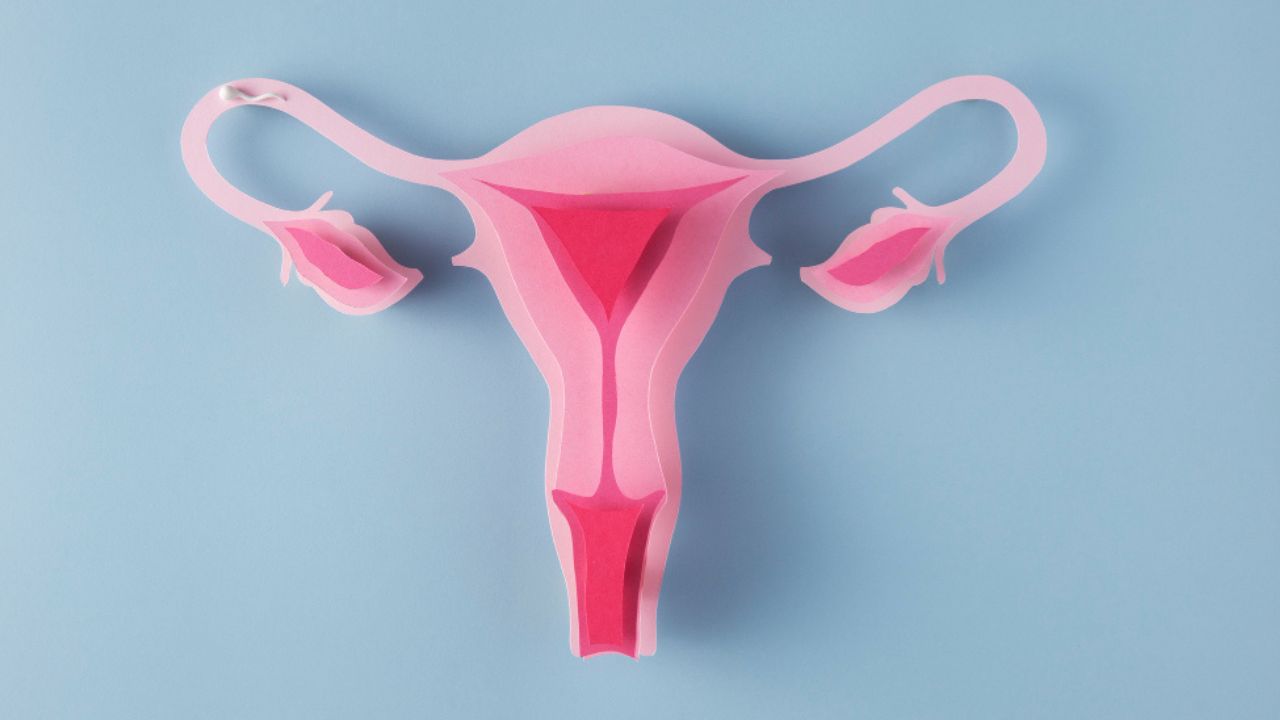
Vaginal agenesis, also known as Mayer-Rokitansky-Küster-Hauser (MRKH) syndrome, is a congenital disorder in which the vagina either develops incompletely or is absent entirely. In these conditions, the uterus or a hypoplastic uterus may also be absent or underdeveloped, among other potential anomalies. These are classified as mullerian anomalies.
This condition can have significant physical, emotional, and social implications for those affected. Women with vaginal agenesis may experience difficulty with menstruation, sexual intercourse, and childbirth.
What is Vaginal Agenesis?
Vaginal agenesis is a rare congenital disorder characterized by the incomplete or absent development of the vagina.
There are two types: complete vaginal agenesis, where the entire vagina is absent, and partial vaginal agenesis, where only a part of the vagina has developed. The prevalence of this condition is estimated to be 1 in 5,000 to 1 in 7,000 females.
What causes vaginal agenesis?
What are the symptoms of vaginal agenesis?
The primary symptom of vaginal agenesis is the absence or underdevelopment of the vaginal canal, which can lead to challenges with menstruation and sexual function. The condition can also have psychological and emotional implications, affecting body image and mental well-being.
Get in touch withDr. Jay Mehta, a renowned gynecologist in Mumbai, India for treatment of Mullerian anomalies and infertility.
How to diagnose Vaginal Agenesis?
Vaginal agenesis is commonly diagnosed in young girls who have not yet started menstruating (primary amenorrhea). This is because the ovaries, which produce the hormones that regulate menstruation, are typically normal in women with vaginal agenesis. As a result, the girl will develop secondary sexual characteristics, such as breast development and pubic hair, normally.
A gynecologist can diagnose vaginal agenesis through a physical examination and a series of tests, including:
- Karyotyping : This test looks at the chromosomes to rule out other conditions that can cause primary amenorrhea.
- Hormonal Testin: This tests the levels of hormones such as estrogen and progesterone.
- Ultrasound : This test uses sound waves to create images of the vagina and uterus.
- MRI: This test uses a powerful magnet and radio waves to create detailed images of the vagina and uterus.
- Genetic Testing: This test can be used to look for genetic disorders that can cause vaginal agenesis.
Book Your Consultation Today With an Vaginal Agenesis Specialist in India – Dr Jay Mehta
Treatment Options of vaginal agenesis
In India, girls with this condition are commonly diagnosed between the ages of 15 and 18 years. The best time to do this surgery is before marriage as soon as the condition is diagnosed. Treatment options vary depending on the individual’s needs and preferences. Some of the treatment options for vaginal agenesis include:
- Vaginal dilation: This is a non-surgical procedure that involves gradually stretching the vaginal opening over time. This can be done using dilators, which are small, tapered instruments.
- Vaginoplasty: This is a surgical procedure to create a vagina. There are a number of different techniques that can be used, and the best option for each woman will vary depending on her individual circumstances. However, the use of skin grafts is no longer recommended due to the risk of complications, such as foul-smelling discharge.
- Laparoscopic surgery with a combined vaginal approach is the most common technique for vaginoplasty. However, if this surgery is performed by surgeons who are not experienced, it may not be successful. This can lead to the need for a redo surgery. Dr. Jay Mehta has performed the maximum number of laparoscopic redo surgeries, and he has a high success rate. He uses peritoneal graft and INTERCEED to achieve excellent results.
- Hormone therapy: In some cases, hormone therapy may be used to help develop the vagina. This is typically used in conjunction with other treatment options.
Dr. Jay Mehta and his team have performed the maximum number of vaginal agenesis surgeries. Women with vaginal agenesis may benefit from a uterine transplant. Consult Dr. Jay Mehta, the Program Director for Uterine Transplant at Global Hospital in Mumbai.
Treatment Options of vaginal agenesis
Is doing MRI compulsory?
In most of the situations in India a basic routine abdomen + pelvic ultrasound is performed on the girl. Should there be a clear suspicion of having a hypoplastic uterus, an absent uterus, and a partially formed or an absent vagina, further imaging in the form of an MRI is routinely warranted.
Further evaluation also needs to be done for the kidney, as associated anomalies of the kidney are common to co-exist with this condition. Routine abdomen + pelvic MRI would cost approximately 6000 rupees in India. Though this is on the slightly expensive side, Dr Jay Mehta and team routinely recommend an MRI for a patient who is suspected to have vaginal agenesis.
Can we women have normal menses?
Majority of these young girls present with a small uterus or hypoplastic uterus or an absent uterus. Despite having fully functional normal ovaries since there is a hypoplastic uterus there is no development of endometrium despite adequate hormonal parameters.
As a result of this even if the surgery is done to create a new vagina which is called as a vaginoplasty these girls do not experience any menses.
Menses can be assured or will resume only after a uterine transparent is done.
Do these women have normal hormones?
As mentioned because the ovary is normal and the ovarian parameters are absolutely normal these girls have all hormonal parameters which are normal. In certain situations an absent vagina is also found in something called androgen insensitivity syndrome.
Androgen insensitivity syndrome can present with abnormal hormonal parameters however the karyotyping in that situation is 46 XY, which is a male karyotype. Routinely girls who present with vaginal agenesis have a type 46XX, which is a female karyotype.
What is the surgical approach of choice?
Dr Jay Mehta and team have performed the maximum number of neo vaginal reconstruction surgeries in India. The team prefers to do a combined approach of vaginal + laparoscopic surgery.
A combination of these techniques along with proper placement of the graft in the form of INTERCEED, which is an OXIDIZED hemi cellulose graft, allows the patient to achieve a vaginal length of approximately 9 cm, allows to maintain excellent patency of the vagina and is excellent for the long term health of the vagina.
Using this technique also ensures adequate length to perform uterine transplant should it be required and the patient be willing for it in the future.
Can a non surgical option like mold be attempted?
In modern day medicine such types of techniques which are very time consuming, have no guarantee of results and are extremely difficult to perform and painful for the patient are no longer performed. After the surgery for creation of a new vagina is done using a combination of vaginal + laparoscopic approach a mold is temporarily placed in this newly created vagina to allow it to stay patent.
What is to be done if the surgery has failed?
Patients who have normally had a failed surgery would then seek the opinion of Dr Jay Mehta. Based on the type and manner in which the previous surgery has been done a repeat surgery is to be attempted. This repeat surgery is typically done laparoscopically.
Most of these patients also require radical vaginectomy. These patients would then benefit from a sigmoid vaginoplasty. Dr Jay Mehta has performed the highest number of sigmoid vaginoplasty in India. A beautiful video of the same is available as a masterclass on YouTube.
What are the complications of this surgery when done by an untrained surgeon?
As depicted in the diagram, organs like rectum and the bladder are extremely close to an absent vagina. As a result of this if there is a surgical trauma, chances of forming a fistula are extremely high in these patients. Repairing the fistula would then require a complex repeat surgery, with adequate diversion and a temporary need to create a stoma.
What is the graft used by Dr Jay Mehta and team?
Since the last 7 years our team has been using INTERCEDE, which is a synthetic oxidized hemicellulose graft, this is used extensively in gynecology as well as in other surgery as an adhesion barrier. The product is extremely safe, marketed and available internationally.
Can a Sigmoid Vaginoplasty achieve a good vagina?
In cases where a repeat surgery is required sigmoid vaginoplasty is the treatment of choice. A sigmoid vaginoplasty is also a commonly done procedure when patients require gender reassignment surgery (GRS). The great thing about the sigmoid is its ability to allow for adequate distension as well as have minimal secretions.
In the long term for patients who require a repeat surgery outcomes with having a vagina from the sigmoid are excellent. We also perform sigmoid vaginoplasty for patients who are post Radiation therapy and desire to have sexual intercourse.
What is the ideal age for getting this surgery done?
The surgery should be performed as soon as the condition is diagnosed. There does not exist any form of alternative medical management to this condition as this is an anatomical defect.
How much bed rest is needed after this surgery?
This is a surgery which is done with a combined approach of laparoscopic surgery + vaginal surgery. Patients are usually discharged within 48 hours of this procedure. There is no recommended bed rest after this surgery.
When can one plan for a Uterine Transplant after this procedure?
After an adequate length of approximately 8 to 10 cm of vagina has been established and has been kept patent for two years. Patients are usually considered for a uterine transplant. We have discussed the entire procedure for uterine transplant in a separate section. Dr Jay Mehta heads the department for Uterine transplant at Global Hospital in Mumbai.

Dr. Jay Mehta
MBBS, DNB—Obstetrics & Gynecology
IVF & Endometriosis Specialist, Laparoscopic Surgeon (Obs & Gyn)
Dr. Jay Mehta is a renowned IVF specialist and fertility-preserving surgeon in Mumbai, India. He is the director of Shree IVF and Endometriosis Clinic, Mumbai. He is a leading laparoscopic gynecologist in India for endometriosis and adenomyosis.
He is a well-known fertility and IVF specialist and also among the few doctors in the country who specialize in embryology and andrology. He operates India’s major cities, including Mumbai, Pune, Chennai, Hyderabad, Bangalore, Ahmedabad, Agra, Delhi etc.
To book an appointment, call: 1800-268-4000 or fill out our contact form

Google Reviews

Ankita Katyal

I am incredibly grateful for Dr. Jay's exceptional support throughout my IVF journey. Dr Jay has been like God sent an Angel for us. From our very first meeting, it was clear that Dr. Jay was not only a highly skilled and knowledgeable professional but also someone who genuinely cared about my well-being.
From my first meeting, he was very clear transparent, and straightforward about my protocol, treatment line, and success rate. After two difficult IVF cycles that failed, I was beginning to lose hope.
However, Dr. Jay’s unwavering encouragement and meticulous care helped me stay positive and focused. Thanks to God and of course to his expertise and dedication, WE FINALLY ACHIEVED SUCCESS!!!!!

Krish A

Dr Jay Mehta is the best Fertility doctor. I am glad to have IVF done with Jay sir.
This unit is very ethical and very honest at work. In my previous IVF cycle, I did not have embryos in Chennai. I was here and Dr and team had told me not to worry. I was given end to end transparency about my embryos and I was lucky to become pregnant in the 1st cycle here, though I was told that the success rate will be about 25 to 30%.
IVF space is competitive, but these guys don't do any Ads on Google. And still if you search, Dr Jay is ranked no.1. I was extremely impressed with that and I am happy that I took a call to travel to Mumbai from Chennai.
I am thankful to the entire team for handling my case nicely. And May God shower the team with his choicest blessings.

Forum Shah

I visited 3 years back for my IVF treatment at that time and also got good treatment with Dr. Jay Mehta … the best part is he would tell me straight away whatever the cause and outcome would be.
This time also I came for Endometriosis treatment n within 3-4 days decided to get operated as there was no looking back as I trust him for his treatment. Thank you Dr once again for the right advice 😊

Deepak Jagadale

Dr Jay Mehta and team are simply excellent people and brilliant outcomes in Fertility services. Very very honest and humble doctor.
Thank you for the valuable guidance during the IVF process and the excellent and no hidden costs during IVF procedure. For middle class people it's a big relief.

Avinash Jain

Dr. Jay Mehta is a result-oriented specialist in his field and the best we could ask for, in a Metro city. His line of treatment for IVF is different from other IVF clinics.
The support provided by doctors and staff as well as all other attending doctors is phenomenal. We are very satisfied and will also highly recommend to others the IVF treatment at Shree IVF Clinic Mumbai.

Vijaya Garg

Dr. Jay Mehta is one of the best gynaecologist doctor of our India. I trust him faithfully and would like to recommend each and every one that don't waste time moving here and there to another doctorand .
I m sharing my experience I wasted my time mand oney by moving from one doctor to other and my problem was unsolved I'm thankful to Dr. Priyanka Shukla mam of trident hospital for suggesting Dr. Jay Mehta sir for my treatment . Now I'm pain-free...Thank you Dr. Jay Mehta sir... you are really my Boley baba shiv shsmbu. I m thankful to all the staff members of Shree IVF hospital
Blogs
Are Mullerian Anomalies a Problem For Infertility?
Uncover how Müllerian anomalies affect fertility in our in-depth blog. From diagnosis to treatment, learn actionable insights for informed decisions on your reproductive health journey.
Müllerian Duct Anomalies: Role in Fertility and Pregnancy
Explore Müllerian Duct Anomalies’ impact on fertility and pregnancy. Discover types, diagnostics, treatments, and antenatal care with expert guidance.
Videos

Absent vagina क्या होता है? | Vaginal Agenesis / MRKH syndrome – Dr Jay Mehta
There are numerous medical conditions that often remain outside the general public’s awareness. One such condition is the absent vagina

Absent vagina के लिए Treatment या Surgery (MRKH syndrome)
For some women with vaginal agenesis, non-surgical methods are a preferable first step. Vaginal dilation therapy is often recommended

