Endometriosis Diet Plan for Pain Relief

Diet does not cure endometriosis.
However, when planned correctly alongside medical treatment, an anti-inflammatory, low-FODMAP diet can significantly reduce symptoms such as chronic pelvic pain, bloating, constipation, abdominal discomfort, and fatigue.
By focusing on antioxidant-rich, fiber-heavy foods, this approach helps manage the underlying inflammation that drives the disease.
This guidance is based on years of clinical experience treating patients with endometriosis and is intended to support, not replace, personalised care from an endometriosis specialist and a certified nutritionist.
Dietary changes should always complement, not substitute, appropriate medical or surgical treatment.
I Have Endometriosis—Will Changing My Diet Actually Help?
This is one of the most common questions patients ask during consultations.
The honest answer is that it can help, but not in the way many online sources suggest.
Endometriosis is a chronic inflammatory condition. Your body is in a persistent state of low-grade inflammation, which worsens pain, disrupts digestion, and affects overall quality of life.
A targeted dietary approach — specifically one that is anti-inflammatory and gut-friendly — can support your body’s response to treatment and reduce the severity of certain symptoms.
However, diet is a supportive tool, not a solution on its own. It works best when used alongside your ongoing medical or surgical management for endometriosis.
If you have been recently diagnosed and are unsure where to begin, consulting a qualified endometriosis specialist is the first and most important step before making any dietary changes.
Can an Endometriosis Diet Plan Really Provide Pain Relief?
Endometriosis is a chronic inflammatory condition. Research suggests that certain foods can either trigger or soothe this inflammation.
A structured endometriosis diet plan for pain relief aims to stabilize the “gut-pelvic axis“—the communication line between your digestive system and pelvic organs.
While diet does not remove endometriotic lesions, it can help manage:
- Chronic pelvic pain and “Endo-belly” (bloating)
- Gaseous distension and constipation
- Systemic fatigue and irritability
However, if you experience deep pain during intercourse (dyspareunia) or bowel movements (dyschezia), this may indicate deep infiltrating endometriosis.
In such cases, diet alone is often insufficient, and you should explore chronic pelvic pain treatment for a more targeted approach.
Why Is There No “One-Size-Fits-All” Diet for Endometriosis?
Every patient’s biological profile is different. Endometriosis is not the same in every woman, which is why a generic diet found online may not work for everyone.
Before adopting the best diet for endometriosis treatment, Dr. Jay Mehta and his team evaluate several important clinical factors:
- Your current body weight and Body Mass Index (BMI)—to balance caloric and nutritional needs
- Ultrasound findings, including Endometriosis Mapping or the presence of bowel nodules
- The stage and severity of your endometriosis
- Your fertility goals and whether you are currently undergoing treatment or planning IVF are aligned with Endometriosis and Fertility Preservation strategies
- The type and severity of symptoms, including pelvic pain, bloating, or fatigue
- Whether deep endometriosis or involvement of organs like the bowel or ureter is present
- Any existing medical conditions such as PCOS, thyroid disorders, anaemia, or IBS
A diet that helps one patient manage bloating may be entirely inappropriate for another patient preparing for in vitro fertilization or recovering from surgery.
This is why a one-size-fits-all approach simply does not work in endometriosis dietary management.
What Is the Connection Between Endometriosis and My Gut?
Many women with endometriosis also experience significant digestive symptoms—bloating, irregular bowel movements, cramping, and gas. This is not a coincidence.
There is a well-recognised connection called the gut-pelvic axis—the bidirectional communication between your digestive tract and your pelvic organs.
When pelvic inflammation is elevated, as in endometriosis, this communication becomes disrupted. The result is a heightened sensitivity in the gut, which explains why so many patients experience digestive discomfort that seems disproportionate to what they eat.
This is precisely why certified nutritionists working with endometriosis patients focus on three combined dietary principles:
- Anti-inflammatory foods — to reduce systemic inflammation
- Antioxidant-rich foods — to counteract oxidative stress linked to endometrial tissue
- Low-FODMAP foods—to minimise gut fermentation and bloating
Understanding FODMAPs is especially important for Indian patients, given how many traditional staples fall into the high-FODMAP category.
Book Your Consultation Today With Dr Jay Mehta—Endometriosis Excision Surgeon in India
What Are FODMAPs and Why Do They Matter in Endometriosis?
FODMAP stands for
- F—Fermentable foods
- O-Oligosaccharides
- D-Disaccharides
- M- Monosaccharides
- A- And
- P-Polyols
These are a group of short-chain carbohydrates that are poorly absorbed in the small intestine.
When they reach the large intestine, gut bacteria ferment them rapidly, producing gas, bloating, and cramping—symptoms that significantly overlap with endometriosis-related discomfort.
Reducing high-FODMAP foods, particularly for a defined period under a nutritionist’s guidance, can help identify specific dietary triggers and reduce abdominal distension.

Which Foods Should I Avoid if I Have Endometriosis—Especially as an Indian Patient?
Endometriosis Diet Chart for Indian Patients: Foods to Avoid
Most certified nutritionists recommend a structured elimination phase lasting approximately 6 to 10 weeks, during which the following commonly consumed Indian foods are reduced or temporarily avoided:
- Gluten & Refined Flour: Wheat (roti, bread, maida, semolina).
- Specific Fruits: Apples and mangoes (high in fructose).
- Lentils & Legumes: Chana, rajma, moong dal, and certain dals that cause gas.
- Aromatics: Onion, garlic (used widely in Indian cooking)
- Dairy Products: Milk and milk-based products.
- Stimulants: Caffeine (Tea/Coffee) and artificial sweeteners
It is important to note that this is not a permanent elimination.
The goal is to identify your personal triggers and then gradually reintroduce foods under a nutritionist’s supervision while maintaining an overall anti-inflammatory dietary pattern.
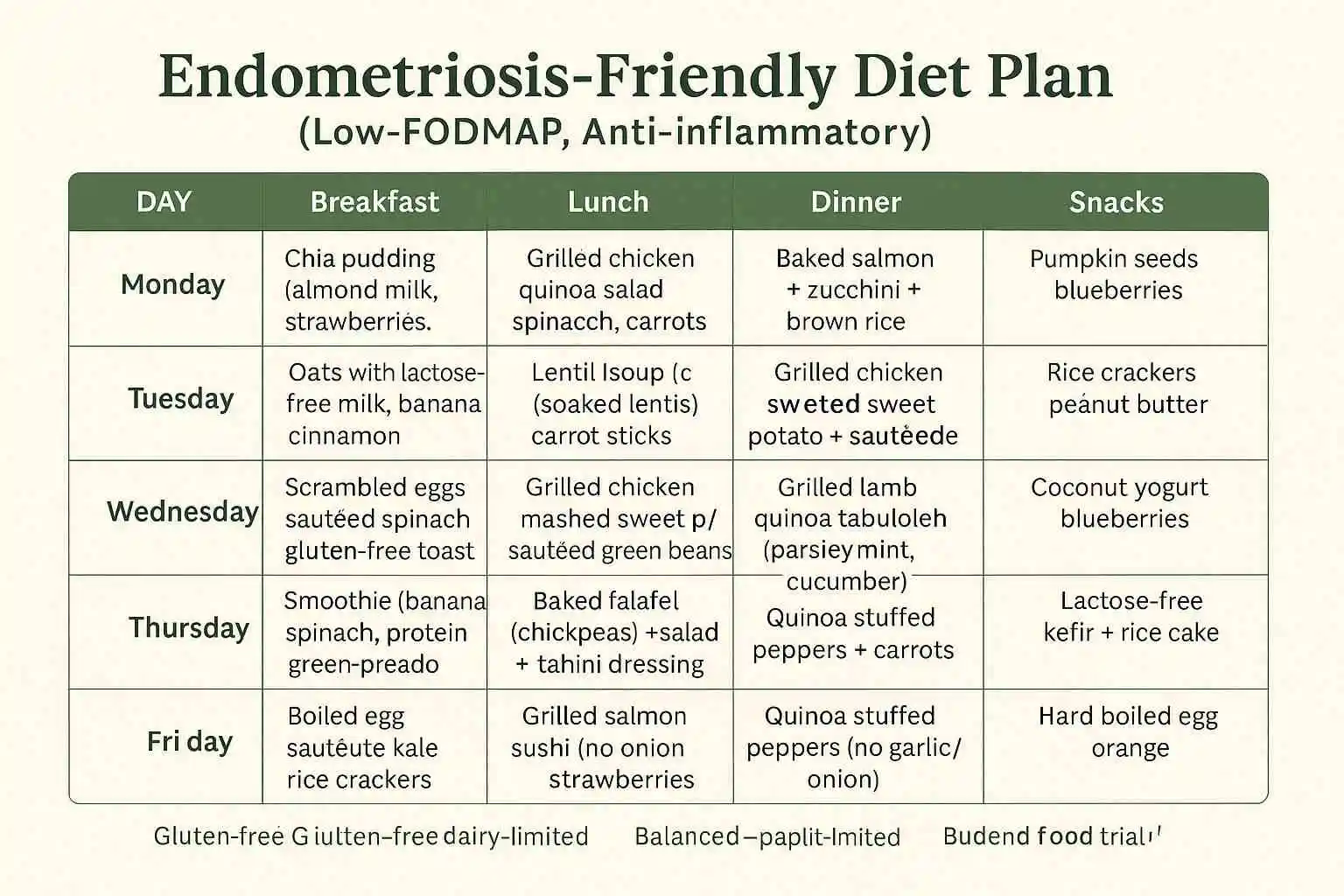
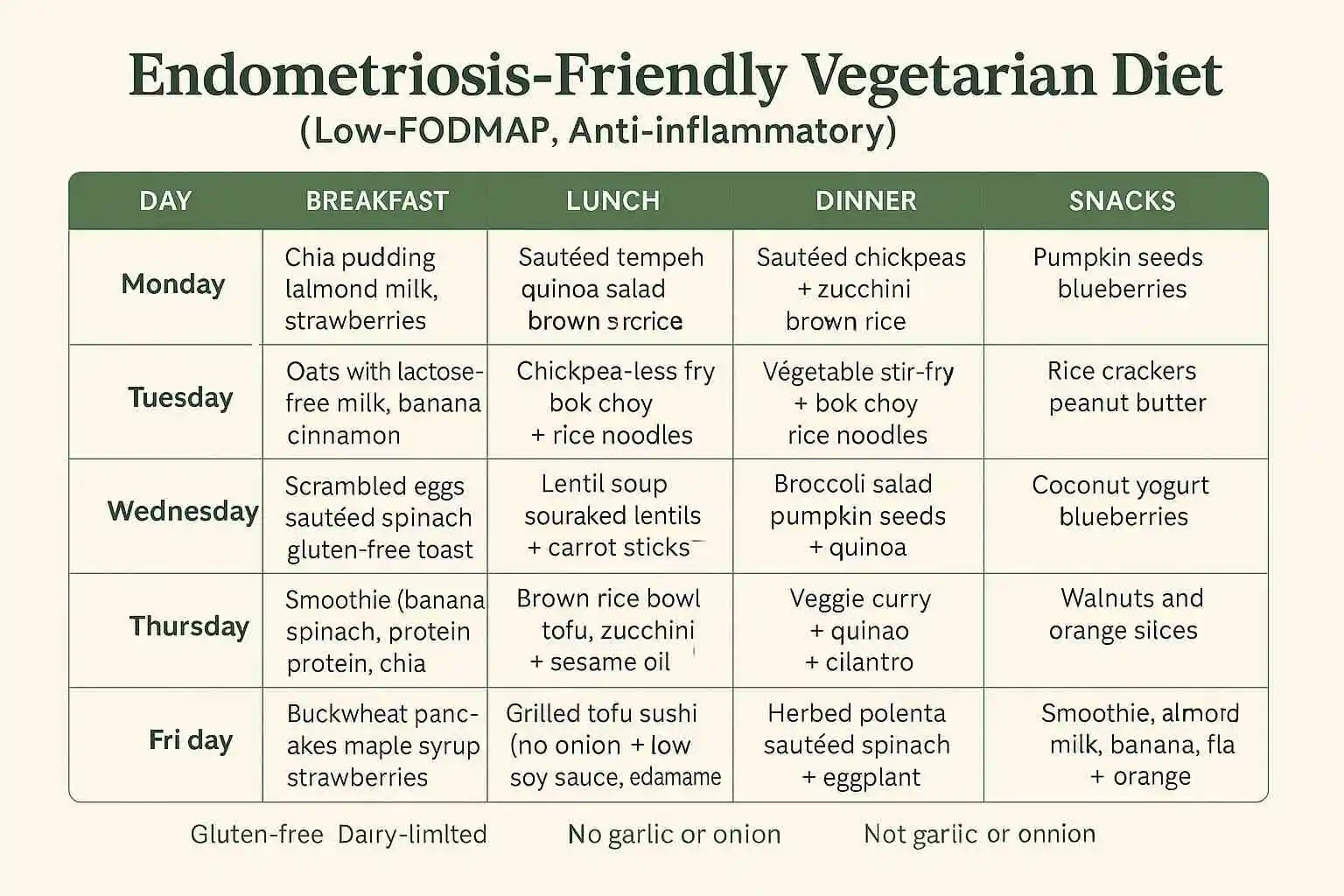
What Foods Should I Actually Eat to Help My Endometriosis Symptoms?
Your certified nutritionist will build a plan around anti-inflammatory, antioxidant-rich, and gut-supportive foods. Some of the most commonly recommended inclusions for endometriosis patients include:
- Chia seeds are rich in omega-3 fatty acids with strong anti-inflammatory properties
- Carrots — a good source of beta-carotene and antioxidants
- Spinach provides iron, magnesium, and folate, which are particularly important for women with heavy periods
- Broccoli and other cruciferous vegetables support oestrogen metabolism and reduce inflammatory markers
- Oats and quinoa are gluten-free grains that provide sustained energy without gut irritation
- Berries such as strawberries are high in antioxidants that reduce oxidative stress
- Bananas (in moderation) — a gentler fruit option with prebiotic properties
This is not an exhaustive list. Your nutritionist will calibrate the exact quantities and combinations based on your calorie needs, work activity level, nutritional status, and treatment phase.
How Long Before I See Any Improvement from an Endometriosis Diet?
This is one of the most frequently asked questions: What is the expected timeline for endometriosis treatment results? — and it requires an honest answer.
Do not expect results within a week. The body takes time to respond to anti-inflammatory dietary changes. Based on clinical experience with a large number of patients, a minimum of 4 to 6 weeks is needed before any meaningful assessment of the diet’s impact can be made.
For patients who consistently follow the plan for approximately 3 months, clinical experience suggests that roughly 50 to 70% of patients report noticeable improvement in the following symptoms:
- Abdominal bloating
- Constipation
- Gaseous distension
- Vague or generalised abdominal pain
- Irritability and mood-related discomfort
These are realistic, evidence-informed expectations—not guarantees. Individual results vary depending on the stage of endometriosis, co-existing conditions, and adherence to the plan.
Will Diet Help if My Pain Is Severe—Like Pain During Intercourse or While Passing Stools?
This is an important distinction that is often overlooked in online endometriosis diet content.
If you experience dyspareunia (pain during intercourse) or dyschezia (severe pain while passing stools), diet alone is unlikely to provide significant relief.
These symptoms typically indicate deeper involvement—such as bowel endometriosis, uterosacral ligament involvement, or pelvic nerve entrapment—which requires dedicated medical or surgical evaluation.
In these cases, dietary changes may still offer some general anti-inflammatory benefit, but they should never be considered a substitute for appropriate treatment.
An accurate diagnosis through endometriosis mapping and clinical assessment is essential before deciding on the right management approach.
If you are experiencing these symptoms, please do not delay seeking specialist evaluation.
Is This Diet Different if I Am Trying to Get Pregnant or Planning IVF?
Yes, and this is a critically important point.
For patients pursuing fertility treatment, including IVF, the dietary approach needs to be adjusted with fertility goals in mind. An endometriosis fertility diet plan is not identical to a general symptom-management diet. Key considerations include:
- Adequate calorie and micronutrient intake to support follicular development and egg quality
- Inclusion of foods that support oestrogen metabolism without excess restriction
- Avoiding nutritional deficiencies that could affect embryo implantation
- Coordinating dietary timing with your treatment protocol
Patients often ask about a specific diet to improve egg quality in endometriosis or a meal plan before IVF.
These plans exist but must be built by a certified nutritionist who is fully informed about your treatment timeline and clinical status.
For patients at Shree IVF and Endometriosis Clinic, dietary referrals are coordinated as part of the overall care plan.
You may also find it helpful to read about endometriosis and fertility preservation to understand how your treatment options and dietary support work together.
What About Hydration? Does That Matter Too?
Yes, significantly. This is a simple but frequently overlooked part of endometriosis dietary management.
Adequate hydration supports kidney function, helps flush inflammatory by-products, aids bowel regularity, and reduces the severity of bloating.
Patients following a low-FODMAP or anti-inflammatory plan must maintain good fluid intake—plain water remains the best option.
Caffeinated beverages, which are dehydrating and pro-inflammatory, should be reduced during the dietary management phase.
What Does It Actually Cost to Follow an Endometriosis Diet in India?
For patients who are considering this approach, here are realistic cost expectations:
| Item | Approximate Cost (India) |
|---|---|
| Initial consultation with a certified nutritionist | ₹6,000 – ₹10,000 |
| Monthly cost of following the recommended diet | Approximately ₹9,000 per month |
These figures will vary depending on your city, the nutritionist’s experience, and your specific dietary requirements.
Many excellent certified nutritional planners practise across India, and your endometriosis specialist can guide you toward an appropriate referral.
Does This Diet Also Help After Endometriosis Surgery?
Yes. Clinical experience shows that the benefits of a structured anti-inflammatory diet extend to patients who are in the post-surgical phase following laparoscopic or other endometriosis procedures.
After surgery, the body is in a healing state, and dietary support can help reduce post-operative inflammation, support recovery, and improve gut function—particularly for patients who have had bowel-related endometriosis treated. In many cases, patients continue the dietary approach as part of their long-term management plan.
If you are considering surgery or have recently undergone treatment, you may benefit from reading about low cost endometriosis surgery and laparoscopic vs. robotic surgery to better understand your options.
Who Should I Speak to About Starting an Endometriosis Diet?
The answer is clear: your endometriosis specialist first, followed by a certified nutritionist.
Do not begin a restrictive diet based on information found on social media or general wellness websites.
Endometriosis is a complex condition, and dietary changes without a clinical context can sometimes worsen nutritional status, affect fertility, or interfere with treatment.
The right pathway is
- Consult your endometriosis specialist—discuss your symptoms, current treatment, and suitability for dietary intervention
- Get a referral to a certified nutritionist with experience in endometriosis or chronic pelvic conditions
- Follow a personalised, evidence-based plan—not a generic template
- Review regularly—your plan should be adjusted as your symptoms or treatment phase changes.
Dr. Jay Mehta, a super-specialist in endometriosis at Shree IVF and Endometriosis Clinic in Mumbai, routinely coordinates dietary referrals as part of a comprehensive management plan for patients with endometriosis across India.
If you are looking for expert, ethical, and personalised endometriosis care, you can reach out to the clinic for a consultation.
FAQs About Endometriosis Diet
– Does diet cure endometriosis?
No. Diet does not cure endometriosis. It is a supportive tool that can help manage symptoms such as bloating, pain, and constipation when used alongside appropriate medical or surgical treatment.
– How long should I follow an endometriosis diet?
An initial structured elimination phase typically lasts 6 to 10 weeks, with a review period thereafter. Many patients continue a modified anti-inflammatory diet long-term as part of their overall management.
– Can an endometriosis diet improve fertility?
A well-planned anti-inflammatory diet may support overall reproductive health, but it is not a fertility treatment. For patients pursuing pregnancy or IVF, dietary plans must be specifically tailored to fertility goals in coordination with your treating specialist.
– Is the low-FODMAP diet the same as an endometriosis diet?
Not exactly. A low-FODMAP approach is one component of an endometriosis-focused dietary strategy. It is specifically used to reduce gut-related symptoms. The full plan also incorporates anti-inflammatory and antioxidant principles.
– Should I avoid all dairy if I have endometriosis?
Dairy is commonly reduced during the initial dietary phase, particularly because it is a high-FODMAP food group. Whether it is eliminated permanently depends on your individual tolerance and nutritional needs, as assessed by your nutritionist.
– How is an endometriosis diet different from a weight loss diet?
An endometriosis diet focuses on reducing inflammation and managing symptoms, not just weight loss. It prioritizes gut health, hormonal balance, and nutrient intake rather than calorie restriction.
– Does an endometriosis diet help regulate periods?
It may help indirectly. By reducing inflammation and supporting hormonal balance, some patients experience more regular cycles and reduced period pain.
– How do I know if the diet is actually working for me?
Improvement is usually seen in reduced bloating, better digestion, and lower frequency or intensity of pain over a few weeks.
– What should I do if I feel weak after starting an endometriosis diet?
Feeling weak may indicate insufficient calorie or nutrient intake. You should consult your nutritionist to adjust your diet instead of continuing with restrictions.
Dr. Jay Mehta is a highly renowned IVF specialist and fertility-preserving surgeon based in Mumbai, India. As the director of the Shree IVF and Endometriosis Clinic in Mumbai, he is recognized as one of India's leading laparoscopic gynecologists for advanced treatment of complex conditions such as endometriosis and adenomyosis. Dr. Mehta and his team have extensive expertise, performing more than 2500 endometriosis cases across India every year at multiple locations. Under his leadership, the Shree IVF and Endometriosis Clinic has consequently become the highest-volume endometriosis and adenomyosis treatment unit in India. Dr. Mehta conducts operations and consultations across India's major cities, including Pune, Chennai, Hyderabad, Bangalore, Ahmedabad, Agra, and Delhi. To book an appointment, call: 1800-268-4000Dr. Jay Mehta
MBBS, DNB – Obstetrics & Gynecology
IVF & Endometriosis Specialist, Laparoscopic Surgeon (Obs & Gyn)
Many Treatments. One Goal.
Caring for Every Patient, Every Day.
ALPA AINCHWAR
Thank you to the best endometriosis surgeon in our India.
Honest and very ethical person.
I want to add one thing, very respectful behavior towards all the patients here.
The only thing is doctor jay is very straight forward.
If he is getting so much work being so straight forward. I can only imagine what will happen if he becomes little sweet and sugary sugary to everyone. But whatever I know him he won’t become like that, kyunki iss Bande ko bhagwaan ka kuch alag aashirvaad hai
Vidhi Mehta
Dr Jay Mehta is a genius at treating endometriosis patients. To the point, no bakwaas. For 13 years I was made to believe I could never conceive naturally, from the age of 19 when I went to a hospital for the first time as an emergency endo patient.
After 2 endo surgeries, 1 failed IVF and a miscarriage here I meet the first doctor who said you will conceive naturally. (Hope). , This was God’s plan, Lord Shiva!!
Thank you Dr. Jay, Dr. Vismay, and the entire team for the hope, treatment, hospitality, and the quickest discharge.
RENUKA RAUT
Great Experience. I have been operated for grade 4 endometriosis. I have never seen a doctor like Jay Sir in my entire life..he is very concerned about his patients..going out of the way to make things possible
Finally, I found an endometriosis specialist after struggling a lot. I am In a safe hand. Each and every staff of this hospital is well-trained and well-managed..highly recommended
Sunitha Suni
He is the god me because im suffering from since 4year pain full period of endometriosis problem im going to so many hospitals any one not identify the problem he is identify and clear endometriosis problem, thanq Dr jay metha sir, Dr Chaitali Rao and ur team Good receiving thanq so much sir ur save my life
md Sohail
Dr. Jay Mehta, what a doctor he is ..hats off.
I really wanted to thank from the bottom of my heart to Dr. Jay Mehta and his dedicated and caring team.
We came from Hyderabad and undergone a major surgery. What a guts he has. I highly recommend Dr Jay Mehta for women who needs a cure for Endometriosis.
Huge thanks to Dr. Chaitali, Dr. Vismai sir and all the supporting staff, nurses and mausis. He is the great doctor and do the best treatment.
Overall very rare kind of personality is Dr.Jay Mehta among the present generation of doctors.
Ankit Jain
I wanted to thank Dr. Jay and his dedicated and caring team at Shree IVF & Endometriosis Hospital at Ghatkopar, Mumbai for the Endometriosis surgery performed. His knowledge of this dreadful disease and its treatment to help thousands of endometriotic women is truly amazing.
He is a gem of a person, explains the problem to patients and their families nicely, and proposes surgical treatment. His caring team also makes the stay in the hospital post-op help to recover quickly.
I highly recommend Dr Jay Mehta for women who need a cure for Endometriosis. He also works brilliantly for IVF and other gynac issues. Kindly check with the clinic and hospital and plan your visit accordingly. They also help with nearby stays for outstation patients. God bless you and give you the strength to continue to work in the noble field.
Blogs

Chances of Getting Pregnant with Endometriosis?
Endometriosis doesn’t always mean infertility. Around 70% of women with minimal to moderate stages conceive without fertility treatment

Can Endometriosis Come Back After Surgery?
Endometriosis may return after surgery, as there’s no guaranteed way to stop it completely. But you can take steps to stay aware and support your health.
Videos

Does Endometriosis Affect the Value of the Anti-mullerian Hormone (AMH)?
Yes, endometriosis can impact your AMH level by damaging the ovaries, fallopian tubes, and surrounding pelvic area.

Pain in Endometriosis
Symptoms of endometriosis include period pain, pelvic and back pain, painful sex, leg pain, and bowel discomfort. Pain can be chronic or intense