Home » Endometriosis » Comprehensive Management of Bowel Endometriosis
Bowel Endometriosis Treatment
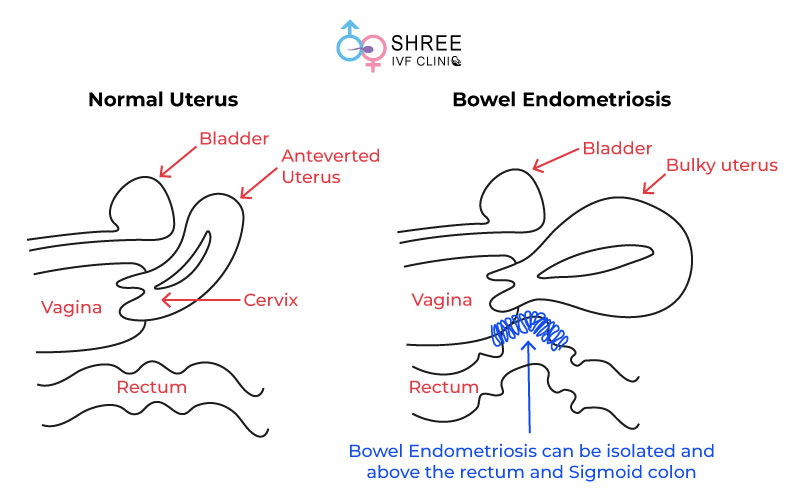
Deep endometriosis of the bowel is a complex and often misunderstood condition.
Bowel endometriosis is different from routine endometriosis. It has a much higher component of fibrosis (thickening and scarring of connective tissue) and a very small component of the glands and stroma.
This disease primarily occurs in the large bowel, especially in the rectum and sigmoid colon, but can also affect the appendix and the area known as the pouch of Douglas. It may be associated with nodular growth of endometriosis in the ureter and parametrium.
Uncommonly, it can also occur outside the pelvis in areas like scar tissue, the umbilicus, and the diaphragm.
Now, as a referral unit for bowel endometriosis across the country & by far the busiest unit in India, especially because we operate at multiple locations like Mumbai, Bangalore, Hyderabad, Delhi, and Chennai. This descriptive review of bowel endometriosis is going to be extremely beneficial to patients who are suffering from this disease or who have typical doubts that are related to this disease.
How can we typically suspect a patient who is having bowel endometriosis?
In India, there are typically a majority of consultants who are not trained in endometriosis. They will typically try to establish a diagnosis based on symptoms where a patient is experiencing dyschezia, which is painful defecation or bleeding per rectum. Unfortunately, these are the symptoms that are typically present in patients who are having an extremely advanced form of endometriosis, where the disease has invaded the mucosa.
If you are a patient, then try and understand that the majority of the time, the endometriosis of the bowel is going to cause you typical symptoms like pain in the pelvis and vague back pain. There could be a certain amount of heaviness while passing stools. They could be altered by habits.
Typically, if you’re having ovarian endometriosis on one side, the possibility that you may have some amount of endometriosis affecting the bowel is going to be approximately 55 to 60%.
However, it is important to understand that if you’re having bilateral ovarian endometriosis, then in that situation, the suspicion for having deep endometriosis, especially endometriosis of the ovary, rises to approximately 95%.
What are the best modalities for the detection of bowel endometriosis?
Modalities have been consistently reported to be excellent modalities for diagnosis of bowel endometriosis. This is an ultrasound, and the second is an MRI here. I am going to be discussing both modalities in detail so that if there is a patient who is viewing this, they can get a great benefit out of reading.
We are a referral unit for endometriosis from across the country, and as a result of this, our team is having a highly specialized unit for detecting endometriosis with the help of ultrasound. This makes us an extremely good unit for identification of bowel endometriosis on ultrasound simultaneously.
Please understand when you do an ultrasound. It is a dynamic testing of the endometriosis, and as a result of which one can easily detect a lot of small nodules as well as detect movement of the uterus in respect to the bow, which is called the sliding sign, and this gives you an added advantage and benefit in planning the proposed surgery.
If, in case, you are a patient who has been referred to do an MRI to detect bowel endometriosis, remember that the best technique to do it is by using gel contrast. Now, this is a contrast that is injected inside the vagina as well as indirectly, and this allows for beautiful delineation of the entire boundary between the vagina and the rectum, thereby allowing us to measure the infiltration of the endometriosis in the axial as well as in the sagittal planes.
Now, in both these situations, it is important for us to understand and evaluate the number of lesions for bowel endometriosis, the depth of invasion of the lesion, the amount of circumference involved, and the size of the lesion.
We have to understand and realize that we, as practicing surgeons, usually end up evaluating even the MRI plates of endometriosis on our own, and this is mainly done by us because our understanding of the disease and correlating it with the symptomatology of the patient has become better over time.
Can any form of medical management be given for bowel endometriosis?
If I answer this question in one line, then the answer is that there is no form of medical management that is currently available for the treatment of bowel endometriosis or, for that matter, any form of deep endometriosis.
This is predominantly because any form of endometriosis, primarily bowel endometriosis, is usually going to be associated with a lot of fibrosis, and because there is a severe amount of fibrosis, there are very limited hormonal receptors that are available, and as a result, medical management simply does not work for this disease.
However, it is very unfortunate to note that in a country like India, there is extremely limited expertise available for the treatment of endometriosis.
The majority of these young girls who are experiencing bowel endometriosis end up going to doctors who do not specialize in the management of the disease at all, and as a result, they end up giving the patient only medical management, which is typically given in the form of an oral antagonist called Elagolix, in the form of dienogest, or the form of GNRH agonists.
Women who are suffering from bowel endometriosis should note that temporary medical management, if continued for a long period, can ultimately give rise to the formation of stricture inside the bowel, and these are situations that may require you to obtain immediate surgery, which has a higher amount of morbidity as well.
Now, since we are a referral unit for bowel endometriosis across our country, what we end up seeing is that the majority of these girls who were having this disease end up coming to us only after 4 to 6 years of having primarily understood that there is this disease.
As a result of this, we end up publishing probably the largest series for the treatment of endometriosis in our country on a consistent year-to-year basis, and this is also one of the reasons why we end up consuming the maximum number of surgical staples in our country.
What are the options for the surgical management of bowel endometriosis?
The type of surgery, which is done for bowel endometriosis, is going to be basically decided upon the size of the lesion, the number of lesions, the location of the lesion, as well as the depth of infiltration.
The vast majority of these patients who are having bowel endometriosis usually will do well with a procedure called bowel or rectosigmoid shaving. This is a procedure where an expert surgeon operates, completely removing the disease right up to the layer of circular muscle in the bowel. In an untrained hand, this is associated with a huge risk of bowel perforation as well.
The bowel endometriotic lesions, which are typically less than 2 cm in size and have an involvement of less than 15% of the circumference, are usually treated with the help of a circular stapler, which gives rise to a DISCOID excision of the bowel.
The bowel endometriotic lesions, which are even larger than that, typically approximately 3 cm in size and occupying approximately 30% of the circumference of the above, are usually the lesions that may require segmental resection & anastomosis of the disease because if any additional procedure is performed instead of that, it can give rise to the formation of a stricture inside this bowel.
A lot of other reconstructive procedures are carried out for lesions that are present at different locations over the intestine, predominantly. This is also associated with a section of the large intestine at multiple locations and the reception and reconstruction of the small intestine.
As a practicing surgeon who specializes in the management of endometriosis, they have to specialize in the treatment and long-term outcomes, as well as the immediate post-operative outcomes of endometriosis affecting the bowel.
What is the follow-up protocol after bowel endometriosis?
Patients are usually monitored with a blood test called CRP, which is done on days 3, 6, 9, 12, and 15, typically after undergoing any procedure for endometriosis of the bowel. Apart from this, all the other clinical sciences for the recovery of the patient are consistently monitored by the team that specializes in the post-operative management of endometriosis.
Once the surgery is performed using a minimally invasive technique, like either laparoscopic surgery or robotic surgery, both of which have almost similar outcomes in these patients, then the patient has to understand that the recovery period is usually 36 to 48 hours, after which the patient is allowed to go back home. We usually allow these patients to carry forward their routine activity, rejoin the office, and travel back to their hometown within 72 hours of the procedure.
Is Removing Bowel Endometriosis Lesions Necessary Before Fertility Treatment?
Studies have consistently demonstrated one thing: if the deep endometriosis is removed before the treatment of fertility, fertility outcomes for the patient are drastically improved because deep endometriotic nodules often give rise to a lot of fibrosis, and it is because of this fibrosis that the contractility of the uterus increases and the other immunological factors that are present due to endometriosis usually give rise to a situation where the implantation rate is drastically reduced.
How to Prevent the Recurrence of Bowel Endometriosis?
The best thing that can be done is to ensure that radical excision, which means complete excision of the lesion of endometriosis, is done by a team that specializes in operating on this disease.
Unfortunately, in a country like India, because patients tend to look out for options that are slightly cheaper compared to the routine options that are available, the majority of the patients get treated by untrained super specialists who only market themselves as specialists in endometriosis, and as a result of which the major majority of the patients whom we end up treating as a referral unit for endometriosis in our country are patients who have been operated at least two times prior.
Can alternative medicines be tried for the treatment of bowel endometriosis?
In a patient who has bowel disease, there is no role for trying any form of alternative management. However, some people have tried alternative medical management for patients at home. The disease has been completely treated by a super specialist, and then it has been tried in order to reduce the rate of recurrence of the disease .
Can one conceive naturally after surgery for Deep Endometriosis of the Bowel?
When an expert performs surgery, this is a fertility-enhancing surgery and plays a role in ensuring that patients who have normal Fallopian tubes can conceive naturally. The difficult aspect of the surgery is to ensure optimal reduction of.
Adenomyosis and endometriosis keep the tubes intact. This requires the expertise of surgeons like Dr. Jay Mehta, who are highly trained and dedicated to the treatment of endometriosis.
Evaluation of the husband is also done for semen parameters before surgery, should the couple be interested in trying naturally post-surgery. A timely surgery helps patients with deep endometriosis in enhancing their fertility outcomes. Testing for AMH (anti-mullerian hormone) is a mandatory thing before such fertility-enhancing surgeries.
Can Deep Endometriosis of the Bowel be associated with a Chocolate Cyst?
Yes, it is common to have ovarian endometriosis, also called a chocolate cyst, present with this.
Do all patients who have Bowel Endometriosis require a Stoma?
No. A stoma is not done routinely at all. For resection of the anastomosis of bowel endometriosis.
Do all patients with bowel endometriosis suspicion need a colonoscopy?
No. Colonoscopy only helps in diagnoses of the lesions that are present in the mucosa, where only a limited amount of lesions actually spread. It’s not indicated.
Is there a big cut on the abdomen to perform this specialized bowel endometriosis surgery?
NO, Dr. Jay Mehta and his team specialize in doing the NOSE technique as well as the complete laparoscopic technique for the bowel resection, wherein the entire procedure, right from resection to stapling, is done with laparoscopic surgery. This ensures extreme safety and rapid recovery at the end of the surgery.
Does all deep endometriosis of the bowel require surgery?
Surgery on 3D laparoscopy is the only treatment option available for these patients. Laparoscopic surgery, when done by an expert, vastly reduces the rate of recurrence to less than 3%. Dr. Jay Mehta and his team have experience operating on more than 500+ cases of deep endometriosis across India every year at multiple locations across India.
Who is the best doctor to consult for deep endometriosis of the bowel?
A patient should choose a doctor who specializes in fertility as well as 3D laparoscopic surgery for endometriosis and adenomyosis; this ensures that the patient can avail complete care under one roof.
Dr. Jay Mehta is the only surgeon in India who also specializes in a complete range of fertility services. This allows patients to make informed decisions about their fertility while choosing a surgery, which in turn greatly enhances their outcomes. This is in stark contrast to places where only the surgeon is available without fertility options.
Can I have a recurrence of Deep Endometriosis of the Bowel?
A disease like deep endometriosis can be removed completely by the best surgical team, as this is a disease in the pelvis.
Dr. Jay Mehta uses a specialized technique of doing this procedure with associated radical excision of the disease as well as complete clearance of the bowel endometriosis; his video on YouTube for the same is very popular. This technique of Dr. Jay Mehta has been well documented as a step-by-step approach for treatment for endometriosis, as well as a masterclass on bowel endometriosis.
Dr Jay Mehta and team have consistently reported recurrence rates of less than 2-3%, which is far less as compared to the routine recurrence of 30% , when the surgery is performed by less experienced surgeons
In conclusion, deep endometriosis of the bowel is a serious condition that requires specialized care and attention. With the right treatment and support, patients can manage their symptoms and improve their quality of life.
If you are one of the people who is facing this problem, consult with Dr. Jay Mehta for any endometriosis treatment in Mumbai, India.
Dr. Jay Mehta is a highly renowned IVF specialist and fertility-preserving surgeon based in Mumbai, India. As the director of the Shree IVF and Endometriosis Clinic in Mumbai, he is recognized as one of India's leading laparoscopic gynecologists for advanced treatment of complex conditions such as endometriosis and adenomyosis. Dr. Mehta and his team have extensive expertise, performing more than 2500 endometriosis cases across India every year at multiple locations. Under his leadership, the Shree IVF and Endometriosis Clinic has consequently become the highest-volume endometriosis and adenomyosis treatment unit in India. Dr. Mehta conducts operations and consultations across India's major cities, including Pune, Chennai, Hyderabad, Bangalore, Ahmedabad, Agra, and Delhi. To book an appointment, call: 1800-268-4000Dr. Jay Mehta
MBBS, DNB – Obstetrics & Gynecology
IVF & Endometriosis Specialist, Laparoscopic Surgeon (Obs & Gyn)
Many Treatments. One Goal.
Caring for Every Patient, Every Day.
Abdul Raheem
The best doctor for endometriosis. I travelled here from hyderabad for my surgery for ovary and bowels endometriosis.
The honesty and the ethics in counselling are what made us choose this doctor. He is an absolute role modal for doctors. We also spoken to other doctors who claim to be endometriosis surgeons . but jay mehta is the best person.
More important it is that sir is very genuine and staff is very genuine.
Vidhi Mehta
Dr Jay Mehta is a genius at treating endometriosis patients. To the point, no bakwaas. For 13 years I was made to believe I could never conceive naturally, from the age of 19 when I went to a hospital for the first time as an emergency endo patient.
After 2 endo surgeries, 1 failed IVF and a miscarriage here I meet the first doctor who said you will conceive naturally. (Hope). , This was God’s plan, Lord Shiva!!
Thank you Dr. Jay, Dr. Vismay, and the entire team for the hope, treatment, hospitality, and the quickest discharge.
RENUKA RAUT
Great Experience. I have been operated for grade 4 endometriosis. I have never seen a doctor like Jay Sir in my entire life..he is very concerned about his patients..going out of the way to make things possible
Finally, I found an endometriosis specialist after struggling a lot. I am In a safe hand. Each and every staff of this hospital is well-trained and well-managed..highly recommended
Sunitha Suni
He is the god me because im suffering from since 4year pain full period of endometriosis problem im going to so many hospitals any one not identify the problem he is identify and clear endometriosis problem, thanq Dr jay metha sir, Dr Chaitali Rao and ur team Good receiving thanq so much sir ur save my life
md Sohail
Dr. Jay Mehta, what a doctor he is ..hats off.
I really wanted to thank from the bottom of my heart to Dr. Jay Mehta and his dedicated and caring team.
We came from Hyderabad and undergone a major surgery. What a guts he has. I highly recommend Dr Jay Mehta for women who needs a cure for Endometriosis.
Huge thanks to Dr. Chaitali, Dr. Vismai sir and all the supporting staff, nurses and mausis. He is the great doctor and do the best treatment.
Overall very rare kind of personality is Dr.Jay Mehta among the present generation of doctors.
Ankit Jain
I wanted to thank Dr. Jay and his dedicated and caring team at Shree IVF & Endometriosis Hospital at Ghatkopar, Mumbai for the Endometriosis surgery performed. His knowledge of this dreadful disease and its treatment to help thousands of endometriotic women is truly amazing.
He is a gem of a person, explains the problem to patients and their families nicely, and proposes surgical treatment. His caring team also makes the stay in the hospital post-op help to recover quickly.
I highly recommend Dr Jay Mehta for women who need a cure for Endometriosis. He also works brilliantly for IVF and other gynac issues. Kindly check with the clinic and hospital and plan your visit accordingly. They also help with nearby stays for outstation patients. God bless you and give you the strength to continue to work in the noble field.
Blogs

Chances of Getting Pregnant with Endometriosis?
Endometriosis doesn’t always mean infertility. Around 70% of women with minimal to moderate stages conceive without fertility treatment

Can Endometriosis Come Back After Surgery?
Endometriosis may return after surgery, as there’s no guaranteed way to stop it completely. But you can take steps to stay aware and support your health.
Videos

Does Endometriosis Affect the Value of the Anti-mullerian Hormone (AMH)?
Yes, endometriosis can impact your AMH level by damaging the ovaries, fallopian tubes, and surrounding pelvic area.

Pain in Endometriosis
Symptoms of endometriosis include period pain, pelvic and back pain, painful sex, leg pain, and bowel discomfort. Pain can be chronic or intense


